Your Gut Is Ground Zero: How Your Microbiome Shapes Your Cancer Terrain
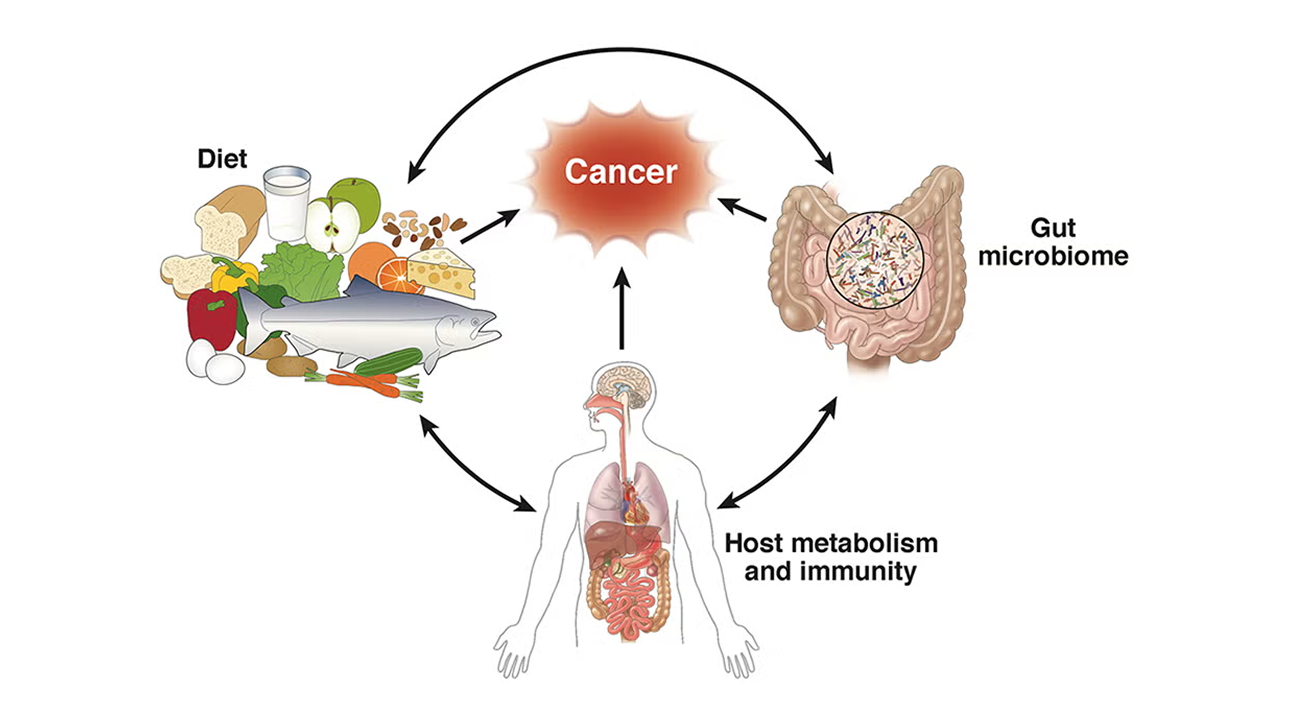

You’ve probably heard the phrase “gut health” thrown around a lot lately — and for good reason. But when it comes to cancer, the conversation goes much deeper than bloating or digestion. Your gut microbiome is one of the most powerful forces shaping whether your body’s internal environment resists cancer or quietly makes room for it.
Think of your body as a garden. Cancer doesn’t just “happen” — it grows in soil that has become fertile for it over time. Your gut microbiome is a huge part of what makes that soil healthy or depleted. And the good news? It’s one of the most changeable parts of your terrain.
What is the “Terrain”?
In integrative oncology, the “terrain” refers to your body’s internal environment — the conditions that either support health or allow disease to take hold. This includes your immune system, inflammation levels, hormones, blood sugar, detoxification pathways, and yes, your gut. Dr. Nasha Winters and Jess Higgins Kelley explore the gut microbiome as a core terrain pillar in The Metabolic Approach to Cancer.
Inside your intestines — mostly your large intestine — live approximately 39 trillion microorganisms: bacteria, fungi, viruses, and more. Together, they form your gut microbiome. Scientists now consider it so important that they call it a “virtual organ.”
When your microbiome is diverse and balanced, it does remarkable things for you every single day:
When the microbiome is out of balance — a state called dysbiosis — these protective functions break down. And downstream, so does much of the rest of your terrain.
“A compromised gut leads to a compromised terrain.”
— Winters & Kelley, The Metabolic Approach to Cancer
Dysbiosis isn’t a dramatic event — it often develops quietly over years through a combination of diet, stress, medications, and environmental exposures. But its effects on cancer risk are anything but quiet.
Leaky Gut and Chronic Inflammation
Your gut lining is only one cell layer thick — a surprisingly thin barrier between the contents of your intestines and your bloodstream. When the microbiome is disrupted, this lining can develop gaps, allowing bacteria and their byproducts to “leak” into circulation. Your immune system responds to this as a constant alarm — and the result is chronic, low-grade inflammation.
This kind of inflammation is now recognized as one of the core drivers of cancer. It feeds several of the “hallmarks” of cancer: helping tumor cells grow, survive, and spread.
The Estrogen Connection
Here’s one that surprises many patients, especially those with breast, ovarian, or uterine cancers: your gut directly controls how much estrogen is circulating in your body.Your liver works hard to package up used estrogen and send it to your intestines for elimination. But certain dysbiotic bacteria produce an enzyme called beta-glucuronidase that essentially unwraps those packages — releasing the estrogen back into circulation. This process is called the estrobolome, and when it’s overactive, estrogen levels rise and risk increases.
Did You Know?
Women with higher beta-glucuronidase activity in their gut have been found to have significantly higher circulating estrogen levels — and greater risk of estrogen receptor-positive breast cancer.
Sources: Kwa M, et al. The intestinal microbiome and estrogen receptor-positive female breast cancer. J Natl Cancer Inst. 2016;108(8):djw029. | Baker JM, et al. Estrogen-gut microbiome axis: Physiological and clinical implications. Maturitas. 2017;103:45-53.
Blood Sugar and the Cancer Fuel Connection
A dysbiotic gut also undermines your blood sugar regulation. And since cancer cells rely heavily on glucose (sugar) for fuel — a phenomenon called the Warburg effect — a gut that promotes insulin resistance is a gut that’s feeding the problem.
The opposite is also true: a healthy, fiber-fed microbiome helps stabilize blood sugar, reduce insulin spikes, and starve cancer cells of their preferred fuel source.
The science on gut health and cancer has exploded in the last decade. Here are some highlights that are particularly compelling in clinical practice:
Colorectal Cancer
A bacterium called Fusobacterium nucleatum — associated with gum disease — has been found in high concentrations within colorectal tumors. Its presence is linked to poorer outcomes and even resistance to chemotherapy. This is a striking example of how the wrong microbes in the wrong place can actively promote cancer.
Breast Cancer
Research has found that women with breast cancer have distinctly different microbiome profiles than healthy women, with lower levels of protective species and higher levels of inflammatory ones. Even the tissue inside breast tumors carries its own microbial signature that tracks with cancer subtype and prognosis.
One of the most exciting recent findings in oncology is that the microbiome can determine whether immunotherapy works. Multiple studies have shown that patients with more diverse gut bacteria — and certain beneficial species — respond significantly better to immune checkpoint therapy (anti-PD-1 drugs like Keytruda and Opdivo).
In a landmark 2018 study published in Science, researchers transferred gut bacteria from immunotherapy “responders” into mice — and those mice then controlled their tumors better. The response was transferred through the microbiome. This is a paradigm-shifting finding.
⚠️ Important for Patients on Immunotherapy
Antibiotics taken within 30–60 days of starting immune checkpoint therapy have been consistently linked to worse survival outcomes in multiple studies. If you are prescribed antibiotics during this window, it is worth having a conversation with your oncology team about timing, necessity, and gut restoration strategies afterward.
The gut is one of the most responsive parts of the terrain. With the right inputs — and by removing the wrong ones — you can meaningfully shift your microbiome within weeks. Here is an approach to gut terrain restoration:
Before you can rebuild, you have to stop tearing things down. The most common disruptors seen in cancer populations include:
Beneficial bacteria are not just passengers — they are dependent on you for their food. The fibers and plant compounds you eat determine which species thrive. A terrain-supportive diet is inherently a microbiome-supportive diet.
The most powerful foods for your gut microbiome include:
Probiotics are live, beneficial bacteria (and sometimes yeasts) that you introduce into your gut — through fermented foods or supplements.
Think of them as reinforcements: microbes you are sending in to rebalance a gut that has been depleted by poor diet, stress, antibiotics, or cancer treatment.
Once they arrive, they get to work:
Postbiotics are the beneficial compounds your gut bacteria produce — the paycheck your gut earns when the good bacteria are doing their job.
The most important postbiotic in cancer care is butyrate — a short-chain fatty acid made when your gut bacteria ferment fiber.
Butyrate does something remarkable on two fronts at once:
For your healthy cells: it is the preferred fuel for the cells lining your colon, actively healing and sealing the gut wall
For cancer cells: it signals them to self-destruct (apoptosis), slows abnormal cell growth, and blocks enzymes called HDACs that cancer cells use to silence your body’s own protective genes
Key nutrients include:
Reducing beta-glucuronidase activity is a priority.
Adequate fiber and bowel regularity — estrogen exits the body in your stool; constipation allows more time for reabsorption
Your gut microbiome is not a side note in your cancer story — it is central to it. It shapes your immune surveillance, your inflammation levels, your hormone balance, your ability to detoxify, and even how well your treatments work.
The good news is that this is one of the most modifiable aspects of your terrain. You have enormous influence over your gut environment through what you eat, how you manage stress, how well you sleep, and the targeted support you choose.
You cannot have a healthy terrain with an unhealthy gut. The two are inseparable.
Key References
Winters N, Kelley JH. The Metabolic Approach to Cancer. Chelsea Green Publishing; 2017. Ch. 6.
Routy B, et al. Gut microbiome influences efficacy of PD-1-based immunotherapy. Science. 2018;359(6371):91-97.
Helmink BA, et al. The microbiome, cancer, and cancer therapy. Nat Med. 2019;25(3):377-388.
Kwa M, et al. The intestinal microbiome and estrogen receptor-positive female breast cancer. J Natl Cancer Inst. 2016;108(8):djw029.
Elkrief A, et al. Antibiotics and outcomes in patients on immunotherapy. ESMO Open. 2019;4(3):e000547.
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011;144(5):646-674.
Baker JM, et al. Estrogen-gut microbiome axis. Maturitas. 2017;103:45-53.
Canani RB, et al. Potential beneficial effects of butyrate in intestinal and extraintestinal diseases. World J Gastroenterol. 2011;17(12):1519-1528.
MamaSweeney Nutrition | Debbie Sweeney, BCHN, FDNp, ONC | Integrative Oncology Nutrition
This blog is for educational purposes only and does not constitute medical advice. Always consult your oncology team before changing your nutrition or supplement protocol.
By Debbie Sweeney, BCHN, FDNp, ONC | MamaSweeney Nutrition Disclaimer: This blog is intended for educational purposes only and does…
Read MoreWritten by: Debbie Dolan Sweeney, BCHN, FDNP, ONC Introduction If you’ve been diagnosed with cancer, you’ve probably heard conflicting…
Read MoreBy Christina Merrill, MSW When someone hears the words, “You have cancer,” life immediately changes. Beyond the medical appointments, treatment…
Read MoreMeaningful conversations with survivors, caregivers, and experts. The CancerBuddy Conversation series brings together diverse voices in candid, uplifting dialogue—offering wisdom, shared experience, and real-life perspective from across the cancer community.
Learn More
With rising cancer rates, our work has never been more important. All donations for the Bone Marrow & Cancer Foundation go to services that directly help cancer patients, survivors, and families. The Foundation relies 100% on private donations. We depend on individual and corporate donors, as we don’t receive government or public funding. We offer innovative ways to contribute, and options for doubling the impact of donations. Thank you for your support, it means so much to so many patients.
Donate